Dr. Paul Lubitz
Dr. Lubitz is an accredited Dermatologist with the Royal College of Physicians and Surgeons of Canada and the American Board of Dermatology. As a skilled and experienced skin specialist, he is equipped to accurately diagnose and treat a full range of skin diseases, including conditions affecting the hair and nails.
Dr. Lubitz is highly trained in the diagnosis and treatment of blood vessel conditions, including varicose, reticular, and spider veins. He offers a range of advanced treatment options including laser therapy, sclerotherapy, and surgical removal. Dr. Lubitz runs a dedicated Vein Clinic for patients with vein concerns in the lower extremities. If you have concerns about blood vessels and would like to explore your options, request a consultation at our Vein Clinic for lower extremity veins or our Cosmetic Clinic for veins located elsewhere on the body.
Please note: Patients wishing to see Dr. Lubitz for medical concerns are required to have a referral from a physician prior to their appointment, typically from their family physician or another accredited healthcare professional. Alberta Health Care (AHC) does not cover all treatments for all medical conditions. The cost of certain medical treatments may be the responsibility of the patient.
Varicose Veins

Veins are responsible for returning blood to the heart once oxygen has been delivered to the body's tissues. When vein walls lose their integrity or pressure within the vessel increases, blood can begin to pool rather than flow efficiently. The result is a gradual stretching of the vein wall that leads to reticular veins and varicose veins — enlarged vessels that often appear purplish or bluish and may protrude visibly beneath the skin, most often in the legs. Pain, swelling, and general discomfort in the affected area are common.
Patients who have varicose veins in the lower limbs carry an elevated risk of developing deep vein thrombosis (DVT), a condition where clots form in the leg veins. If a clot breaks free, it can travel to the lungs or brain with potentially life-threatening consequences.
A number of factors are known to increase the likelihood of developing vein disease, including genetics, advancing age, pregnancy, prior limb injuries, obesity, cardiovascular disease, chronic illness, and occupations or habits that involve prolonged sitting or standing with legs crossed.
When vein disease progresses to a moderate or severe stage, it can restrict a person's mobility and contribute to a condition called stasis dermatitis. This raises the patient's vulnerability to skin infections, chronic ulcers, and compromised wound healing.
Compression stockings are often recommended for patients with reticular or varicose veins as a way to support healthier blood return from the lower extremities.
Dermatologists receive specialized training in the identification and management of vein disease. A consultation at Primaris Dermatology can help determine the type and severity of vein disease, establish what can be done to slow its progression, and outline the treatment paths best suited to each individual patient.
Why You Need Treatment
Varicose and reticular vein treatment can be for medical or cosmetic reasons, often both. It is important to remember that varicose veins and damaged reticular veins are a medical concern, particularly if left untreated, as they usually worsen over time and contribute to increased patient morbidity. In addition to causing pain and discomfort, they can cause swelling, skin rashes, redness, and sores and be a source of infections. Severe varicose veins may lead to deep vein thrombosis (DVT), a serious medical condition requiring immediate medical attention. Early diagnosis and treatment by a dermatologist trained in vein disease, such as Dr. Lubitz, will promote improved skin and vein health and contribute to greater mobility later in life.
Surgical stripping is a well-established technique for treating large varicose veins, particularly those located in the upper thigh and groin. While still appropriate in select cases, it typically involves a more significant recovery period. Advances in treatment now allow many of these vessels to be addressed with less downtime using endovenous laser ablation or ultrasound-guided foam sclerotherapy.
Sclerotherapy is the most widely used treatment for reticular and varicose veins. A liquid or foam solution is injected into the affected vein, causing it to close off and gradually be absorbed by the surrounding tissue over time.
Laser-based treatments offer a minimally invasive approach to vein disease. A YAG laser is used for reticular veins, while endovenous laser ablation (EVLA) is used for varicose veins. Both work by sealing damaged vessels and encouraging blood flow to redirect through healthier veins.
Spider Veins or Spider Vessels
Spider veins, medically known as telangiectasia, are tiny dilated vessels that become visible near the surface of the skin. They appear most frequently on the legs, face, chest, and hands. In most cases they are painless and represent a cosmetic concern rather than a medical one, though they can bleed if injured. Sclerotherapy and laser therapy are both effective treatment options.
Acne

Acne vulgaris is one of the most common skin conditions seen in clinical dermatology, affecting a large proportion of teenagers and a significant number of adults. During adolescence, more severe forms of acne tend to affect males more frequently. In adulthood, however, women are more commonly affected and often contend with the condition for longer periods.
What Does Acne Look Like?
Acne can take many forms, from blackheads and whiteheads to inflamed pimples and deep, painful cysts. The condition originates within the hair follicles and oil glands, where abnormal cellular activity causes oil ducts to become blocked. When bacteria accumulate within the blocked gland, inflammation follows, producing the characteristic lesions associated with acne.
The psychological toll of acne is well documented. Patients frequently report feelings of self-consciousness and reduced confidence, and in adolescents particularly, social withdrawal and anxiety are not uncommon. When acne goes untreated or is managed incorrectly, permanent scarring can develop, creating lasting effects on self-esteem that persist long into adulthood.
Your Treatment Options
The encouraging reality is that acne responds well to treatment in the vast majority of cases. The most important factors are an accurate diagnosis and early intervention to prevent long-term skin damage. At Primaris Dermatology, our dermatologists bring extensive experience in managing all forms of acne and acne scarring. Available treatments include oral and topical medications, laser therapy, light-based treatments, chemical peels, and medical-grade cosmeceutical skincare. Our team will work with you to find the right combination approach for your skin.
Actinic Keratosis

Actinic keratosis is among the most frequently encountered pre-cancerous skin conditions, developing on areas of skin that have sustained cumulative sun damage over time. Without appropriate treatment, these lesions carry the potential to progress into non-melanoma skin cancers, including squamous cell carcinoma and basal cell carcinoma. Early identification and management by a dermatologist is strongly recommended.
Alopecia

Alopecia is the medical term for hair loss arising from an underlying medical cause. While most forms of alopecia do not present a direct health risk, patients who lose significant scalp coverage face increased UV light exposure, which can raise the risk of scalp skin cancer. Beyond physical health, many patients seek treatment because of the emotional weight that comes with premature or irregular hair loss.
Your Treatment Options
Hair loss is not a single condition. There are several distinct types, including androgenic alopecia, alopecia areata, scarring alopecia, and telogen effluvium, each with its own set of causes and corresponding treatments.
Alopecia areata is an immune-mediated condition in which the body's immune system attacks its own hair follicles, resulting in hair loss that may be temporary or permanent. It can affect the scalp or any other hair-bearing area of the body. Treatment options include topical and oral medications, cortisone injections (intralesional and intramuscular), and immunotherapy to stimulate regrowth.
The most effective treatment strategy depends on the specific type of alopecia and the individual patient's circumstances. Our dermatologists at Primaris Dermatology are trained to evaluate and manage the full range of hair loss conditions.
Contact Dermatitis
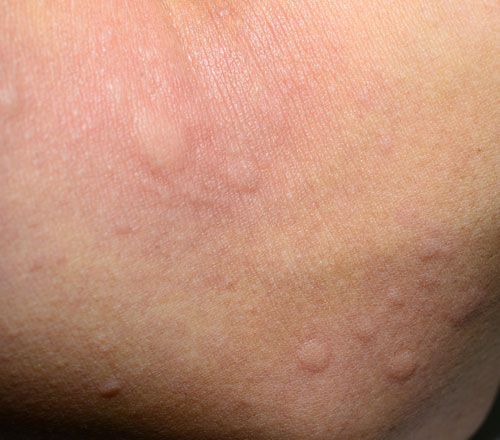
Contact dermatitis is a reactive skin rash caused by exposure to an external substance. It falls into two categories, both of which can occur in the same patient at the same time:
-
Allergic Contact Dermatitis occurs when the skin reacts to a substance the patient is allergic to, such as latex, hair dye, nail products, or cosmetics.
-
Irritant Contact Dermatitis develops after prolonged or repeated contact with substances that are physically harsh on the skin, such as cleaning agents or industrial chemicals.
Environmental Factors
Climate can be a contributing factor. The notably dry conditions in Alberta are a known contributor to irritant contact dermatitis for many residents. A familiar everyday example is diaper rash, which results from a baby's skin being in extended contact with moisture and irritants in a soiled diaper.
Dilated Pores

Over time, skin pores can become persistently enlarged, forming what is medically referred to as a dilated pore of Winer. These are non-harmful lesions, but patients frequently seek treatment when they appear on the face or other cosmetically sensitive areas.
Your Treatment Options
For individual lesions, treatment options include retinoid-based topical therapy, punch grafting, and surgical excision. For patients with more widespread areas of dilated pores, broader cosmetic approaches such as fractionated CO2 laser treatment and chemical peeling techniques can produce meaningful improvement.
Hair Disorders

The range of hair disorders seen in dermatology is broad. They may be inherited or acquired, and can involve the way hair grows, the structure of the hair shaft itself, or be secondary to infection or systemic disease.
Conditions treated in this category include hair loss in its various forms, excessive hair growth including hypertrichosis and hirsutism, structural abnormalities such as brittleness and breakage, colour changes, and scalp conditions tied to systemic diseases including psoriasis, lichen planus, lupus erythematosus, contact dermatitis, and seborrheic dermatitis.
Accurate diagnosis is the foundation of effective treatment, and our dermatologists at Primaris Dermatology are trained to evaluate and manage the full spectrum of hair disorders.
Hyperhidrosis

Hyperhidrosis is the clinical term for sweating that significantly exceeds what the body requires for temperature regulation. It is not a medically dangerous condition, but its impact on daily life can be considerable. Many patients experience chronic anxiety, social discomfort, and a meaningful reduction in self-esteem as a result. The condition can affect the underarms, hands, feet, face, head, neck, and chest.
Neuromodulators to Treat Excessive Sweating
Neuromodulators, including Botox, represent a well-established and effective treatment option for hyperhidrosis. When administered to the affected areas, they work by interrupting the nerve signals responsible for triggering sweat glands. For many patients, the results are dramatic and genuinely life-improving. Speak with our team at Primaris Dermatology to find out whether neuromodulator treatment is right for you.
Lupus Erythematosus

Lupus is an autoimmune disease in which the immune system mistakenly targets the body's own tissues, causing inflammation and damage that can affect multiple organs, including the skin.
Signs and Symptoms of Lupus
Symptoms vary widely between patients but frequently include persistent fatigue, joint pain or swelling, unexplained fever, and skin rashes that intensify with sun exposure. Kidney involvement is also common in certain forms of the disease.
Types of Lupus
-
Systemic lupus erythematosus (SLE) is the most severe form, with the potential to affect many body systems simultaneously.
-
Discoid lupus erythematosus (DLE) primarily affects the skin, producing raised, red lesions that typically appear on the face and scalp. These can become thick and scarring over time. Hair loss, thinning, or breakage may also occur.
-
Additional variants include subacute cutaneous lupus, bullous lupus, lupus profundus, drug-induced lupus, and neonatal lupus, each of which is less common.
Melasma

Melasma is a pigmentation disorder that causes brown or grey-brown patches to develop on the skin, most commonly on the face. It occurs more frequently in women and in individuals with medium to darker skin tones. Hormonal influences, particularly estrogen, are a primary trigger, and sun exposure significantly worsens the condition. It can also appear on the neck, chest, and arms.
Caring for Your Skin with Melasma
Consistent sun protection is one of the most important things a melasma patient can do. Daily sunscreen application and wearing a hat when outdoors help prevent existing patches from darkening further. Melasma is particularly common during pregnancy, where it is sometimes referred to as the mask of pregnancy. Hormonal contraceptives containing estrogen can also trigger or worsen the condition.
Several other pigmentation disorders share a similar appearance to melasma, making professional diagnosis important. While melasma occasionally fades on its own, it more often becomes permanent and progressive without treatment. A dermatologist can provide an accurate diagnosis, appropriate patient education, and a targeted treatment plan.
Treatment Options
Hydroquinone is a topical agent that reduces melanin production in the skin, progressively lightening affected areas. Prescription-strength formulations prescribed by your dermatologist are generally more reliable and potent than over-the-counter alternatives.
Tretinoin and corticosteroids are topical medications that support the skin-lightening process and are often used in combination with hydroquinone. A compounded all-in-one cream containing all three ingredients is frequently more effective than applying each product separately.
Additional topical agents such as azelaic acid and kojic acid may be recommended either on their own or as part of a broader treatment protocol.
For patients who require more intensive intervention, cosmetic treatment options include TCA chemical peeling, the Obagi Skin Restoration Protocol, and carefully selected laser treatments. Laser therapy for melasma requires particular caution, as certain devices can trigger a rebound darkening effect. Our team at Primaris Dermatology will guide you toward the safest and most appropriate options for your skin type.
Psoriasis

Psoriasis is a chronic immune-mediated skin disease that affects over one percent of Canadians. It causes the body to produce new skin cells at an accelerated rate, faster than the old cells can be shed. The result is a buildup of skin on the surface that produces the scaly, inflamed patches characteristic of the condition. Psoriasis can also affect the nails, leading to pitting, thickening, discolouration, or separation from the nail bed.
Affected Areas
The scalp is one of the most commonly affected areas, where psoriasis may cause scaly patches, persistent flaking, and itching. Inflammation, repeated scratching, aggressive treatments, and the psychological stress of living with a chronic skin condition can all contribute to temporary hair loss. Psoriasis can also involve the joints, causing inflammation, pain, reduced range of motion, and in some cases irreversible joint damage.
Treatment Options
Psoriasis can be managed effectively with a range of topical, systemic, and light-based therapies. Because the condition presents differently from patient to patient, early and accurate diagnosis is key to selecting the most appropriate treatment. Our dermatologists at Primaris Dermatology are experienced in assessing all presentations of psoriasis and are trained in the latest treatment protocols.
Rosacea

Rosacea, formally known as erythrotelangiectatic acne rosacea, is a chronic inflammatory skin condition that primarily affects the face. It is characterized by persistent redness, visible dilated blood vessels, heightened skin sensitivity, and acne-like breakouts. The nose, cheeks, and chin are the most frequently involved areas. Rosacea is particularly common among individuals with fair skin, especially those with Northern European or British ancestry. The condition worsens progressively if not managed, and in some men, advanced rosacea can cause a bulbous thickening of the nasal tissue known as rhinophyma.
Caring for Skin Affected by Rosacea
Avoiding known triggers is central to managing rosacea effectively. Common aggravating factors include sun exposure, extreme heat or cold, strong winds, alcohol, hot drinks, and spicy foods. Because rosacea can closely resemble several other skin conditions, an accurate diagnosis by a dermatologist is critical. Delayed or incorrect diagnosis often leads to unnecessary discomfort and a reduced quality of life. Understanding personal triggers is an important part of keeping the condition under control.
Treatment Options
Managing rosacea typically involves a combination of lifestyle adjustments and medical treatments tailored to the specific aspects of the condition affecting each patient. Our team at Primaris Dermatology will work with you to identify your triggers and build an effective, personalized management plan.
Tinea Infections
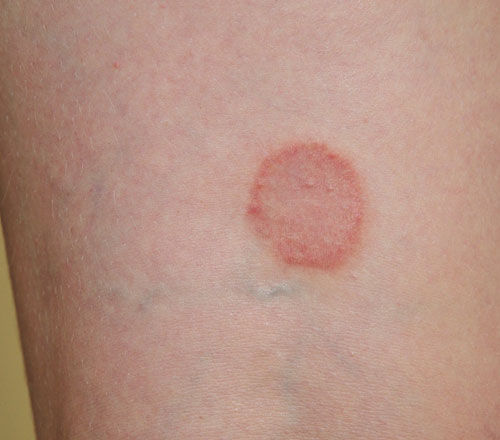
Tinea is a fungal infection caused by a group of organisms known as dermatophytes. Transmission occurs through direct contact with the fungus or its spores. On its own, tinea is not a dangerous condition, but it can cause persistent itching and discomfort. In vulnerable populations, including young children, older adults, and individuals with weakened immune systems or pre-existing health conditions, an untreated tinea infection can become complicated by secondary bacterial or yeast infections.
Types of Tinea Infection
Ringworm appears as a red, circular rash on the skin. Despite its name, it has no connection to any parasitic worm and is entirely fungal in origin.
Athlete's foot affects the skin between the toes and may also spread to the soles and sides of the feet, causing itching, burning, and peeling. It is commonly acquired from damp communal surfaces such as shower floors, pool decks, or saunas.
Jock itch develops in the groin area and produces an itchy, burning rash that can be persistent if left untreated.
Because tinea infections can mimic other skin conditions, including psoriasis, contact dermatitis, and granuloma annulare, an accurate clinical diagnosis is important. When properly identified by a dermatologist, tinea infections can be resolved effectively with prescription topical medications available through Primaris Dermatology.